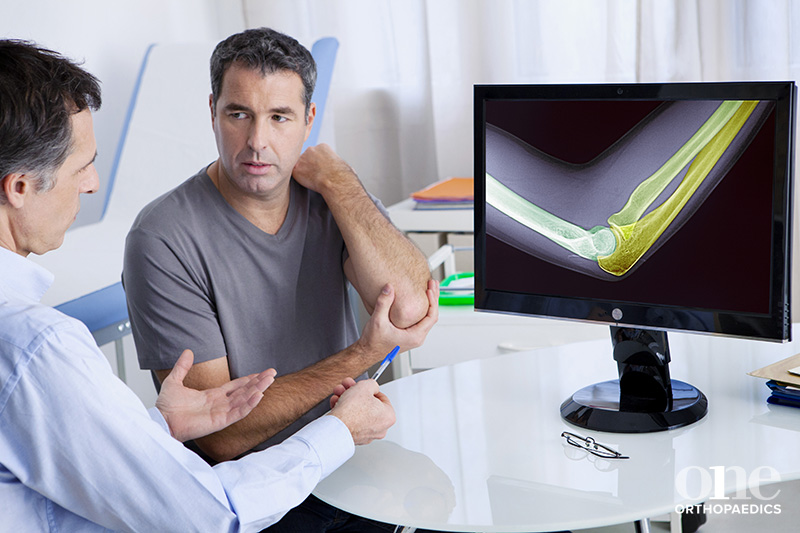
What is elbow arthritis ?
Arthritis of the elbow is a degenerative condition, which develops when the cartilage of the elbow joint becomes damaged or is worn away over time.
Why does elbow arthritis occur?
Arthritis in the elbow is unusual due to the shape of the bones and robust stabilising ligaments. The elbow joint can therefore be subject to a large amount of force before it becomes unstable. More commonly, arthritis affects weight-bearing joints including the hip and knee.
Most patients diagnosed with arthritis in the elbow have a history of a fracture or dislocation or they have an inflammatory arthritis such as rheumatoid. When bone gets damaged or worn away, the bone tries to heal itself by producing extra bone. The bone forms irregularly, causing bone spurs known as osteophytes. These osteophytes often form around joints affected by arthritis, causing pain and stiffness which restricts movement in the joint.
Activities that overload or overuse the joint, particularly common in throwing athletes, also cause degenerative wear and tear.
Elbow arthritis symptoms
The main symptoms are increasing pain, stiffness and swelling in the elbow. These symptoms become worse following periods of continuous activity.
Elbow arthritis can cause irritation to the ulna nerve. In the later stages, patients may notice numbness in their ring finger and small finger. This can be caused by elbow swelling or limited range of motion in the joint. The ulnar nerve or ‘funny bone’ is located in a tight tunnel on the inner side of the elbow. Swelling in the elbow joint can put increased pressure on the nerve, causing tingling. If the elbow cannot be moved through its normal range of motion, it may stiffen into a position where it is bent. This can also cause pressure around the nerve to increase.
How is elbow arthritis diagnosed?
There are three articulations within the elbow joint and it is important that your consultant identifies the exact cause of the pain and stiffness coming from your elbow. You will be asked a series of questions to establish whether you have any risk factors for arthritis and determine the severity of your symptoms. They will also carry out a detailed examination of your joints. In most cases the diagnosis is confirmed with an x-ray, but occasionally further tests or scans may be required.
Elbow arthritis treatment
The best course of treatment for elbow arthritis depends on the part of the joint affected, your general health, your activity levels, and the severity of your symptoms. Conservative options would almost always be tried before surgical options are considered. As there are three articulations within the elbow, your consultant should identify exactly which aspect of the joint is affected prior to initiating treatment. There could be a number of other factors contributing to arthritis, and these also need to be eliminated before treatment is prescribed.
Non-surgical treatment
Early stage arthritis is most commonly managed with pain relief, modification of activities and physiotherapy. Physiotherapy can help to delay onset and severity of stiffness in the joint.
Steroid injections can also be used to treat arthritis symptoms. Although the effects of injections are temporary, they can provide significant pain relief, until symptoms progress enough to need surgical intervention.
Platelet-rich plasma (PRP) injections are being used more and more where conservative treatment is not effective. A solution is extracted from the patient’s own blood, rich in growth factors which aid tendon healing.
Surgical treatment
If symptoms continue and progress, surgery may be indicated. Arthritis can be seen on x-rays when there has been significant wear or damage to the joint surfaces. If the wear or damage is limited, arthroscopy (keyhole surgery) can offer a minimally invasive surgical treatment. It may be an option for patients with earlier stages of arthritis.
The One Orthopaedics team specialists

Anthony Hearnden
Consultant Orthopaedic Surgeon FRCS (Tr&Orth), Shoulder, Elbow, Hand and Wrist